DIETARY SUPPLEMENTS
Découvrez 08 - Slim
Your ally for a slimmer figure and healthy weight

Journal
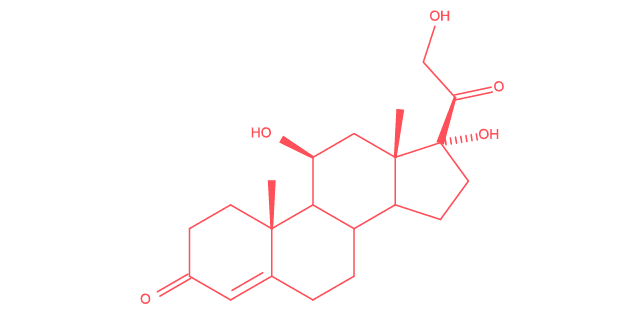
Cortisol is a hormone produced by the adrenal glands in response to signals from the brain, through what is known as the hypothalamic–pituitary–adrenal (HPA) axis.
Often referred to as the “stress hormone,” cortisol is, in reality, essential to the body’s overall balance.
It plays a central role in:
— energy regulation
— blood sugar control
— immune function
— sleep–wake cycles
Under normal conditions, cortisol follows a precise circadian rhythm:
it peaks in the morning to promote alertness, then gradually declines throughout the day to allow the body to wind down.
This finely tuned regulation is a cornerstone of how the body adapts to daily demands and environmental stressors [1,2].
Cortisol itself is not the problem.
It is a hormone of adaptation.
In response to acute stress, it allows the body to:
— mobilise energy quickly
— increase focus and alertness
— prepare for immediate action
This “fight or flight” response is entirely physiological.
The issue arises when this response becomes chronic.
Under repeated stress—whether emotional, professional, metabolic, or inflammatory—cortisol levels can remain elevated, or become dysregulated altogether.
Recent research shows that prolonged disruption of the HPA axis is associated with deep metabolic, immune, and inflammatory imbalances [3].
Chronically elevated cortisol is not just a feeling of stress.
It has measurable biological consequences:
— increased blood glucose levels
— enhanced fat storage, particularly abdominal
— disrupted sleep patterns
— low-grade chronic inflammation
— reduced insulin sensitivity
Recent studies confirm cortisol’s central role in metabolic regulation and its contribution to insulin resistance, particularly in the context of chronic stress [4,5].
Cortisol also directly affects immune function, leading to both immune suppression and inflammatory dysregulation [11].
The skin is particularly sensitive to hormonal fluctuations.
When cortisol remains elevated over time, it can lead to:
— increased skin inflammation
— impaired barrier function
— heightened sensitivity
— breakouts
— dullness
— accelerated skin ageing
Recent data show that chronic stress reduces skin lipid levels, weakens the skin barrier, and increases transepidermal water loss [7].
Cortisol also impacts wound healing, immune defence, and inflammatory pathways in the skin, contributing to visible imbalance [6,8,9].
Emerging research further links chronic stress and cortisol exposure to accelerated cellular ageing in the skin [13].
From a Cellular Nutrition® perspective, cortisol should be understood as a signal.
It reflects the overall state of the body.
Chronically elevated cortisol rarely exists in isolation.
It is usually part of a broader biological context:
— persistent fatigue
— chronic inflammation
— microbiome imbalance
— metabolic dysregulation
— disrupted sleep
Chronic stress has also been linked to increased gut permeability and systemic inflammation via the gut–brain axis [10].
In other words, cortisol is not just a stress hormone.
It is a marker of a system under strain.
Balancing cortisol does not rely on a single intervention.
It requires a coherent, system-wide approach.
The most well-established levers include:
— restorative, consistent sleep
— an anti-inflammatory, whole-food-based diet
— stable blood sugar regulation
— effective stress management (movement, breathwork, recovery)
— support for the gut microbiome
These factors are interconnected and determine the body’s ability to return to hormonal balance.
Integrated approaches are now recognised as the most effective way to restore physiological cortisol regulation.
Within this framework, N°0 OPTIMAL was formulated to address the core mechanisms involved in stress and energy regulation.
Its approach is multi-dimensional:
— modulation of the stress response (notably through adaptogens such as Rhodiola)
— support of neurotransmitters involved in focus and resilience
— enhancement of mitochondrial energy production
— support of the gut–brain axis
Adaptogenic plants like Rhodiola rosea have been shown to improve stress resilience and help regulate cortisol response [14].
At the same time, restoring energy production and digestive balance helps reduce the underlying signals that sustain dysregulation.
Cortisol is neither the enemy nor a simple “stress hormone.”
It is a central regulator of biological balance.
When properly regulated, it supports energy, alertness, and adaptability.
When dysregulated, it becomes a key driver of metabolic, inflammatory, and skin-related imbalances.
Understanding cortisol means recognising that stress is not just a feeling.
It is a measurable biological state that profoundly shapes how the body functions.
And it is by acting on underlying signals—not just symptoms—that lasting balance can be restored.
[1] Tsigos C, Chrousos GP. Hypothalamic–pituitary–adrenal axis and stress. Endocrine Reviews. 2002.
https://academic.oup.com/edrv/article/23/4/457/2424115
[2] Chu B et al. Physiology of the stress response and HPA axis. StatPearls. 2024.
https://www.ncbi.nlm.nih.gov/books/NBK541120/
[3] Nunez SG et al. Chronic stress, HPA axis dysfunction, and immune imbalance. 2025.
https://pubmed.ncbi.nlm.nih.gov/41155288/
[4] Sic A et al. Chronic stress, cortisol dysregulation and metabolic health. 2024.
https://pmc.ncbi.nlm.nih.gov/articles/PMC11431196/
[5] Chao AM et al. Stress, cortisol and appetite-related hormones. 2017.
https://pmc.ncbi.nlm.nih.gov/articles/PMC5373497/
[6] Knezevic E et al. Cortisol, neuroinflammation and chronic stress. 2023.
https://pmc.ncbi.nlm.nih.gov/articles/PMC10706127/
[7] Stress-Induced Changes of the Skin: A Narrative Review. 2025.
https://pmc.ncbi.nlm.nih.gov/articles/PMC12681996/
[8] Stress and Skin: Mind–Body Therapies Review. 2021.
https://pmc.ncbi.nlm.nih.gov/articles/PMC8480446/
[9] Role of stress in skin diseases. 2023.
https://pubmed.ncbi.nlm.nih.gov/38128623/
[10] Madison AA et al. Stress, inflammation and gut permeability. 2023.
https://pmc.ncbi.nlm.nih.gov/articles/PMC10867428/
[11] Immunology of stress: effects of cortisol on immune function. 2024.
https://pmc.ncbi.nlm.nih.gov/articles/PMC11546738/
[12] Stress and telomere shortening. 2021.
https://pubmed.ncbi.nlm.nih.gov/34736994/
[13] Stress mediators, aging and skin. 2023.
https://pubmed.ncbi.nlm.nih.gov/38906383/
[14] Panossian A, Wikman G. Effects of adaptogens on the central nervous system and stress. Pharmaceuticals. 2010.
https://www.mdpi.com/1424-8247/3/1/188